Channels
Special Offers & Promotions
Tumour Analysis Following Surgery could Provide Breakthrough in Predicting how well Cancer Patients Respond to Drug Treatment
University of Leicester and Medical Research Council researchers lead study to monitor effectiveness of drugs on cancer patients
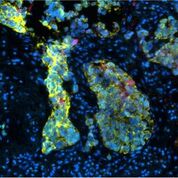 University and MRC researchers have developed a new platform for assessing anti-cancer drug efficacy in lung cancer that is more reflective of patient response than previously used model systems.
University and MRC researchers have developed a new platform for assessing anti-cancer drug efficacy in lung cancer that is more reflective of patient response than previously used model systems.
The platform relies on the derivation of ‘explants’ from tumour tissue obtained fresh from surgery and treatment of these samples ex vivo with anti-cancer drugs.
The platform has the potential to significantly reduce drug attrition rates and increase the success of anti-cancer drugs in the clinic, thus improving patient benefit.
A novel approach developed by researchers from the University of Leicester and the MRC Toxicology Unit could help to predict how well patients respond to drugs designed to fight various forms of cancer.
The team has developed a patient-relevant pre-clinical platform called ‘explants’, whereby tumour samples are taken from cancer patients immediately following surgery and drug responses are then assessed in situ.
The ‘explant’ approach is cheap, quick, and reproducible and has already given results that are more predictive of patient outcome than other methods.
The study, which was led by Professor Catrin Pritchard and Dr Howard Pringle from the University of Leicester Cancer Research Centre and Professor Marion MacFarlane, who is based within the MRC Toxicology Unit at Leicester, applied the ‘explant’ approach to lung cancer.
They found that the different cell types within a tumour are retained intact and that the way in which the tumour ‘explants’ respond to drugs predicts how well individual patients respond in the clinic.
Professor Pritchard explained: “Despite the huge level of investment into the development of new anti-cancer drugs by academia and the pharmaceutical industry, most do not deliver patient benefit in the clinic.
“We carried out this study to test whether our ‘explant’ approach gives patient-relevant data with regard to standard-of-care chemotherapy and provide strong evidence that this is indeed the case for lung cancer.
“If incorporated into drug development procedures, then the ‘explant’ platform has an opportunity to make a huge contribution to the anti-cancer drug development pipeline.”
Professor MacFarlane added: “This work is important as it will reduce the attrition rates of cancer drug development and improve the efficiency and speed with which anti-cancer drugs are incorporated into the clinic to give patient benefit. This will also substantially reduce the costs of developing novel anti-cancer drugs.
“We are very excited by the potential of our platform and have already expanded our approach to other cancer types such as breast cancer, mesothelioma and colorectal cancer with excellent results in each of these disease types.”
In recognition of the potential of the platform, Cancer Research UK Therapeutic Discovery Laboratories previously co-funded method development and following this successful pilot study the team has now completed a research agreement with both Cancer Research UK Therapeutic Discovery Laboratories and LifeArc to test a range of novel anti-cancer drugs, attracting investment totalling >£500K.
Tim Hammonds, Deputy Director of Drug Discovery at Cancer Research UK Therapeutic Discovery Laboratories, said: “Access to clinical tissues for our drug discovery projects should provide vital information on the mechanisms and possible application of new therapeutics. We are delighted to be working in this collaboration.”
Dr Justin Bryans, Executive Director, Drug Discovery at LifeArc, said: “We are very excited about this collaboration. The ability to test experimental drugs against explants will provide valuable information and enable us to expedite the discovery of new cancer therapies. In addition, if we can use this platform to inform oncologists of the appropriate treatment for their patients then this could transform the way we treat cancer.”
This has allowed the establishment of a ‘Cancer Explant Facility’ located in the University’s Robert Kilpatrick Clinical Sciences Building at the Leicester Royal Infirmary Site. This facility is also being supported by the University’s Leicester Drug Discovery and Diagnostics Centre (LD3), and the Leicester Precision Medicine Institute (LPMI).
Alasdair Gaw, the Commercial Director of both LD3 and LPMI, commented: “The development of this pre-clinical platform is a great example of how a collaborative approach based on excellent scientific research can positively impact clinical practice to provide patient benefit and typifies why Leicester is a leading centre for precision medicine.”
The work was funded through the award of an MRC Doctoral Training Grant that allowed the appointment of Ellie Karekla, a PhD student who worked as part of the research team. Additional funding, for consumables and overheads, was provided by the MRC Toxicology Unit, following on from a previous MRC Development Gap Fund Award to Professor MacFarlane and also by funding from the MRC Confidence in Concept Award (institutional translational funding).
The Leicester Experimental Cancer Medicine Centre, funded by NIHR and Cancer Research UK, provided support in the form of tissue collection nurses.
Barry Sharp, John Pugh and Helen Reid from the Centre for Analytical Science from Loughborough University contributed to the assessment of drug delivery within explant samples.
more about university of leicester
Media Partners